The ‘surgical never events’ task force and its impact
In 2014 I chaired the NHS England surgical never events task force, and authored our final report “Standardise, educate, harmonise: Commissioning the conditions for safer surgery”
The report of the never events task force was followed by implementation of the National Safety Standards for Invasive Procedures (NatSSIPs) in 2015. This was an initiative we proposed under our ‘standardise’ theme, and it was implemented by way of a Patient Safety Alert which is supposed to mandate action by providers of NHS care.
Since then, a review by the Healthcare Safety Investigation Branch of the ten ‘never events’ it had investigated resulted in a recommendation to strengthen the NatSSIPs and to reduce the degree of permitted local variation. I comment below on why we originally proposed that the NatSSIPs should be implemented locally through Local Safety Standards for Invasive Procedures (LocSSIPs).
HSIB also made a number of other observations that are suggestive of how the other two aspects of our report, ‘educate’ and ‘harmonise’ have disappointingly gone unnoticed.
Understanding surgical ‘never events’
We were asked to look at the reasons for the persistence of three never events in surgery (listed below); to consider whether the World Health Organisation checklist was helping to reduce them; and to make recommendations about what NHS England, with its responsibilities for commissioning, could do to reduce them further.
The three never events we looked at were wrong site surgery (which includes operating on the wrong site, carrying out the wrong procedure, and operating on the wrong patient); wrong prosthesis (for example, the wrong size components in a replacement hip); and retained foreign object (the most frequently retained foreign object is surgical swabs, but this also includes surgical instruments).
The term “Never Event” appears to have been coined around 2001 by Ken Kizer, former CEO of the US National Quality Forum. He used it to refer to particularly egregious errors (such as wrong site surgery) that should never occur, not least because it was already known how to prevent them. The NHS in England went on to adopt the concept in April 2009 following Lord Darzi’s report High Quality Care for All (DH, 2008).
HSIB and other commentators have been critical of the nomenclature of never events. Their argument is that several of the NHS’s designated never events are not strictly ‘never events’ because there are not sufficiently strong safety barriers in place to guarantee they could not arise. Our concern as a task force was not whether wrong site surgery was aptly named a never event (although we did not support the name). Our focus was what could be done to prevent these events.
While surgical never events occur in only a tiny fraction of the total number of operations (around 1 never event per 20,000 operations, or 0.005%) there were 265 reported cases in NHS funded care in 2012 – 2013. This is one for each working day. That is 265 events in which patients suffer harm, need extra care, experience bewilderment and anxiety, and lose trust in their care providers; 265 events that have serious consequences for staff including emotional turmoil, loss of confidence and capability, and impact on their employment; and 265 events that require providers to investigate, report, and face financial penalties.
The task force included expert surgical practitioners (surgeons, anaesthetists, operating department practitioners, and representatives from nursing and midwifery), patients and patient advocates with intimate knowledge of surgical harm, and academic experts in fields such as human factors, safety in high risk industries, incident reporting and analysis, and use of the World Health Organisation checklist. We carried out an online survey to which over 600 people responded, sharing their views as practitioners, patients, managers, lawyers, and safety experts. We searched the international literature for data and insights. And we carried out interviews with patients and staff who had experienced surgical never events.
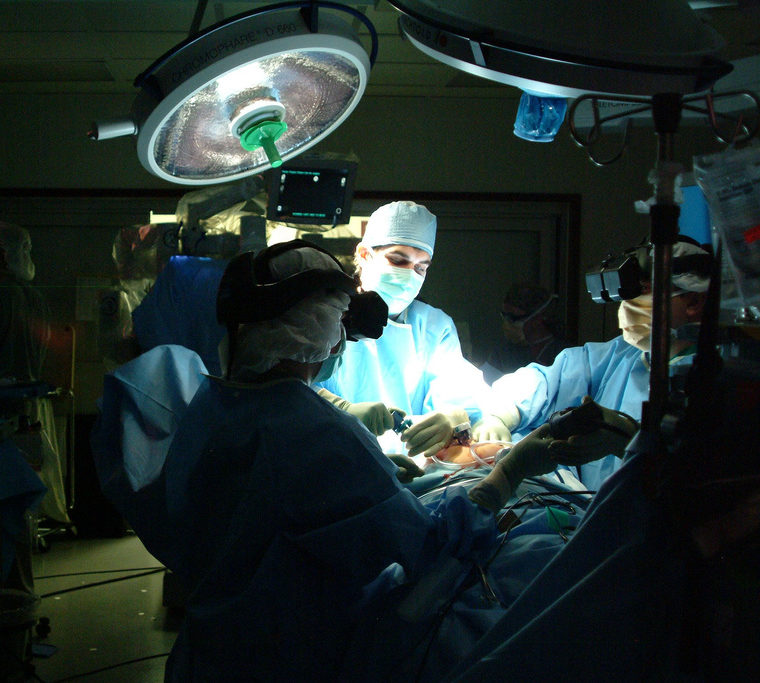
Surgery by Army Medicine CC BY 2.0
Where did all this get us?
A consistent and compelling message emerged: there was no single cause underlying the occurrence of the never events we reviewed. Never events are almost always the result of multiple sources of error.
Sources of error consistently recognised in the research literature are:
- intrinsic complexity of surgical technologies & procedures, allied to the need to accommodate individual patient variation & preferences;
- significant variation in professional approaches to safety related processes (e.g. swab counting) leading to muddle, confusion and failure to act in accordance with unfamiliar protocols;
- failures in planning, organisation and co-ordination even where resources and personnel are not an issue (e.g. operating lists that are changed at the last minute, patient order being altered during operating lists);
- time pressures and the use of ‘work arounds’ to manage work pressure;
- unplanned events and distractions that disrupt work flow;
- general communication failures, which may be viewed as symptomatic of the enormous challenge in communicating what needs to be communicated in all of the above circumstances
Respondents to our own consultation also highlighted risks created by:
- poor professional behaviour
- chronic lack (or poor utilisation) of resources, creating an unsafe operating environment.
So what can be done about it? As H.L Menken famously observed, for every complex problem there is an answer that is clear, simple, and wrong. Our answer was, I think, clear. But it was not simple.
We chose to propose a three-pronged strategy, aware that the success of this strategy would rest on each prong being treated as equally important. This was not going to be easy for the NHS, which at the time was already running to keep up with its recent reorganisation, the many recommendations of the Francis Report, the imperative to redesign care to meet the needs of an older population, and the need to reduce costs while maintaining quality. But a simple solution – if wrong – would be far worse than a challenging one.
What has become apparent since our report was published was that while the ‘standardise’ message was heard (and resulted in the introduction of the National Safety Standards for Invasive Procedures) the other two part of the report have been largely overlooked.
The three prongs: standardisation, education, and harmonisation.
The first element was standardising generic operating environment procedures (for example, swab and instrument counts, prosthesis verification and list management). We proposed that professionals should take the lead role in developing and continuously reviewing National Standards that set out broad principles of best practice, and suggest a range of acceptable means of implementing best practice. Providers would be required to embed these National Standards in their own local processes by developing, in collaboration with their staff, Local Standards. The National Standards should be incorporated into the NHS Standard Contract, meaning that they apply to all NHS funded care, whether carried out by NHS Trusts or private providers.
This system of profession-led National and Local standards was intended reduce variation and promote best practice, whilst still providing scope for local innovation and reinforcing responsibility at provider level.
HSIB has since suggested that the NatSSIPs should be a single set national standard, in order to further reduce unwarranted variation. We deliberately chose not to pursue this course of action for three reasons:
- imposing a single set of national standards would be a ‘command from the top’ without need for real consideration of safety by the teams responsible for it – our aim was to start a conversation in every surgical team in the country about the core national standards and what if any variation was justified
- different surgical specialties present different challenges – a standard requiring indelible ink site marking would work for skin but would need a different approach in dentistry, and this needs to be developed by knowledgeable teams in the specialty
- without variation there cannot be improvement – a single set of national standards would choke innovation
The second element is systematic education and training, including for those managing operating environments. Our recommendations proposed that surgical safety be addressed in undergraduate level qualifications for doctors, nurses, and operating department practitioners; in postgraduate training, including the NHS Management training programme; and in Trust provision for continuing professional development. Addressing surgical safety would mean – amongst other things – teaching practitioners about human factors, and how human-human and human-technology interactions affect safety.
Further recommendations addressed the responsibilities of Higher Education England, the General Medical Council, Deaneries and medical Royal Colleges for ensuring that curricula and training programmes incorporate appropriate safety training; and of the Care Quality Commission for reviewing the adequacy of provider training.
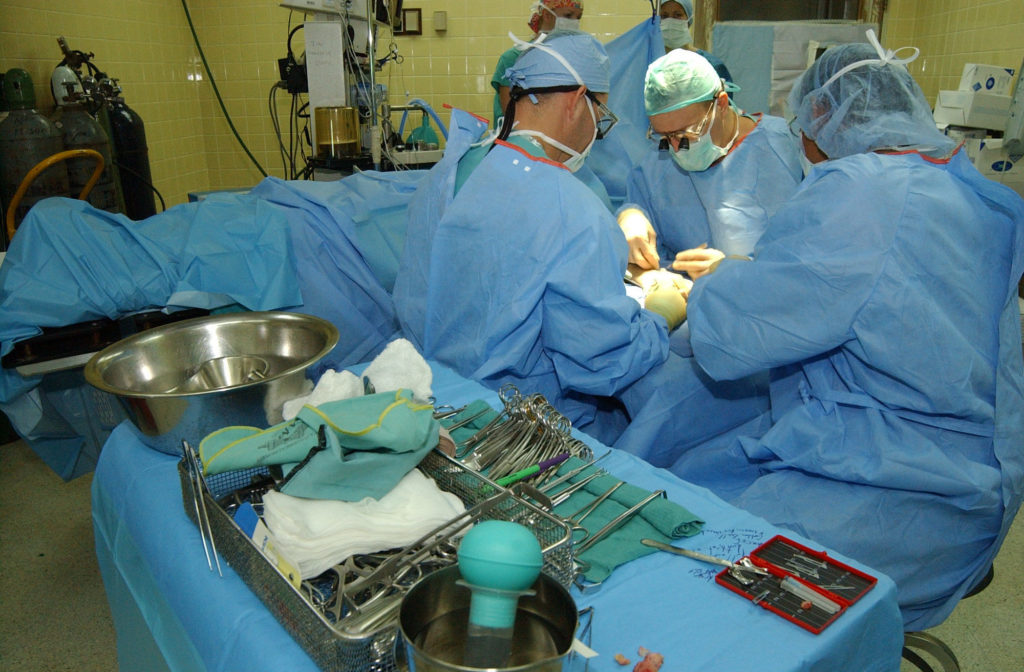
Surgery by Army Medicine CC BY 2.0
The final element was harmonising activity to support patient safety in hospitals. The Berwick report and our own are equally clear that professional and organisational incentives must align to support safety and the development of a just culture. Examples of our recommendations under the theme of harmonisation include: NHS England and Clinical Commissioning Groups to impose penalties only where provider response to a never event, including patient support, is assessed as ineffective (thus avoiding creating a deterrent to reporting); Responsible Officers to ensure that appraisal for revalidation includes evidence of activity concordant with Local Standards; and the NHS Litigation Authority to make clear how National Standards and Local Standards contribute to defining the required legal standard of care.
Looking after patients and professionals following adverse events
The most overlooked part of our report was our argument that never events are not over when a patient leaves the operating theatre. The task force looked carefully at the support that patients and their loved ones need when never events – and other serious incidents – happen. Professional-ethical duties and the statutory duty of candour mandate that patients are told promptly and honestly when something has gone wrong. But being open is not enough.
When things go very wrong patients are entitled to candour, and much more than candour. They also need caring and compassionate support, a credible and independent investigation into what happened, a thoughtful approach to restitution, and proper accountability.
Just as importantly, professionals involved in incidents need appropriate support. In the NHS, thousands of healthcare professionals will go to work today committed to making people better and, if they can’t make them better, giving them comfort. By this evening, someone will unintentionally have done their patient harm. The very opposite of what they aimed to do, this can be devastating. How professionals then deal with this awful turn of events affects patients, colleagues, and the systems we design to keep patients safe. So professionals need help to manage the situation well, not only for their own benefit, but also to build a safer culture of care.
You can download the full version of Standardise, Educate, Harmonise or its Summary from my virtual filing cabinet.
Image by Phalin Ooi via flickr CC: by 2,0

